What Does a Registered Psychologist Actually Do? A Straightforward Guide
Rod Mitchell, MSc, MC, Registered Psychologist
Key Highlights
Registered Psychologists complete specialized training in assessment, diagnosis, and evidence-based treatment across diverse populations.
Psychologists use comprehensive psychological testing to clarify diagnosis and personalize treatment approaches effectively.
Extensive training develops the clinical judgment needed to navigate treatment resistance, complex comorbidities, and ethical challenges in practice.
First sessions focus on history-gathering and rapport, then collaborative goal-setting determines whether CBT, EMDR, or other modalities fit best.
When someone tells me they're considering therapy, one of the first questions they ask is "what does a Registered Psychologist do?" – and I understand why there's confusion.
Mental health professionals have overlapping titles, and it's genuinely difficult to know who does what. In my years of practice, I've seen clients initially seek counsellors or psychiatrists when they actually needed the specialized assessment and evidence-based treatment Registered Psychologists provide, which delayed their progress.
This article explains:
What Registered Psychologists actually do in practice
What therapy sessions look like beyond abstract descriptions
The specialized training that distinguishes this profession from other mental health careers
Table of Contents Hide
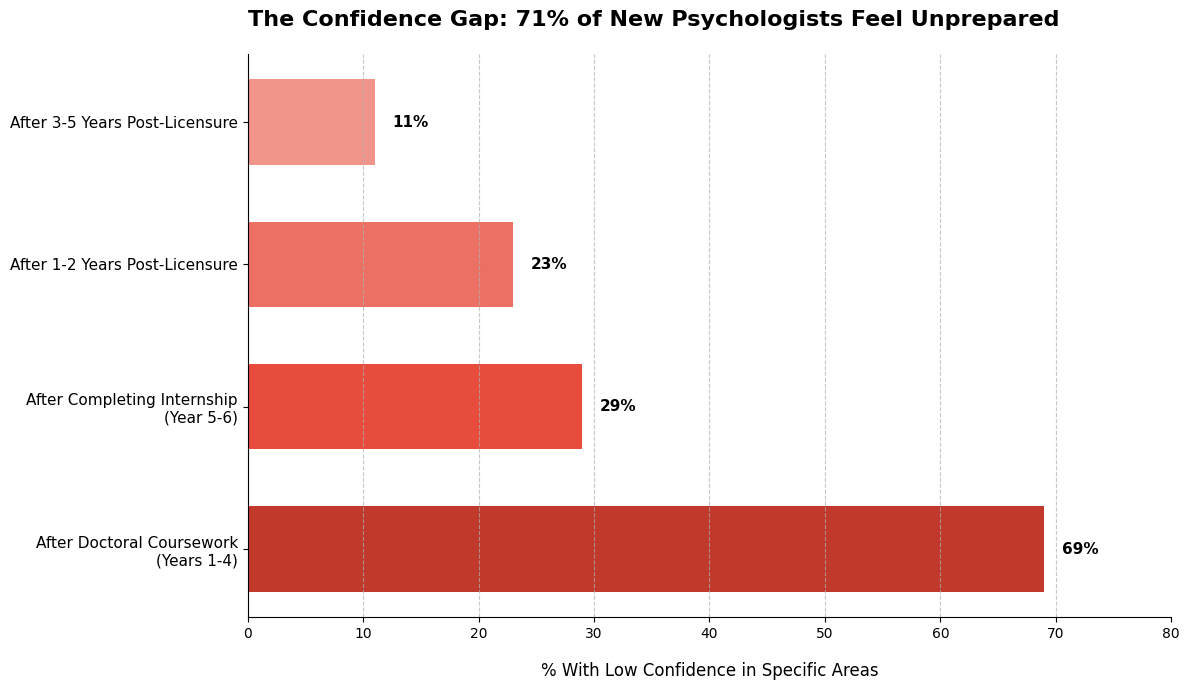
Clinical psychology training is rigorous, but confidence lags behind credentials. 29% of graduates still don't feel adequately prepared for independent practice.
The gaps are most pronounced in high-stakes areas: 51% report low confidence treating personality disorders and 38% feel unprepared for suicidal crises, despite these being common presenting issues.
What Is a Registered Psychologist?
Registered Psychologists are regulated mental health professionals who specialize in the assessment, diagnosis, and evidence-based treatment of psychological disorders and emotional difficulties. In Alberta, this title is protected by law and regulated by the College of Alberta Psychologists (CAP), ensuring practitioners meet rigorous standards of education, training, and ethical practice.
This profession requires specialized graduate training that distinguishes it from other mental health roles.
Training and Credentials That Matter
In Alberta, Registered Psychologists hold a graduate degree (master's or doctoral) in psychology from an accredited program. Unlike some American jurisdictions that require doctoral-level training, Canadian provinces recognize master's-level practitioners as fully qualified Registered Psychologists.
Before becoming fully registered, candidates must complete supervised practice hours under a Registered Psychologist. In Alberta, this typically involves 1,600 hours of supervised experience for master's-level graduates, with requirements varying based on the nature of the graduate program. During this period, practitioners hold the title of Provisional Psychologist.
The training emphasizes psychological assessment, differential diagnosis, and treatment of mental health conditions using evidence-based approaches.
What Sets Registered Psychologists Apart
| Profession | Can Diagnose Mental Disorders? | Psychological Testing Training | Typical Training |
|---|---|---|---|
| Registered Psychologist | Yes, using DSM-5-TR | Extensive | Graduate degree + 1,600 supervised hours |
| Psychiatrist | Yes, medical model | Minimal | Medical degree + psychiatry residency |
| Counselling Therapist (Alberta, unregulated) | No | Varies (no minimum standard) | No regulated requirements currently |
The ability to conduct comprehensive psychological assessments represents a key distinction. Registered Psychologists receive specialized training in cognitive testing, personality assessment, and psychological evaluation. This expertise allows them to clarify diagnoses when presentations are complex or when multiple conditions overlap.
In Alberta, Counselling Therapists are not yet a regulated profession - meaning anyone can currently use the title regardless of training. The government announced in March 2024 that the College of Alberta Psychologists would take on regulatory oversight of counselling therapists, but implementation has stalled.
Until regulation is in place, the key distinction remains: Registered Psychologists are accountable to a regulatory college, can conduct formal psychological assessments, and can diagnose mental health conditions, whereas unregulated counselling therapists have no such oversight or diagnostic authority.
Who Registered Psychologists Work With
Registered Psychologists treat individuals, couples, and families across the entire lifespan. You might see a Registered Psychologist for:
Depression, anxiety, or trauma
Relationship and family conflicts
Behavioural problems in children
Life transitions and adjustment issues
Chronic health conditions affecting mental health
Complex diagnostic questions
Research shows that broadly-trained Registered Psychologists achieve consistent treatment outcomes across different age groups and presenting problems, with effectiveness rates equivalent to age-specialized providers for most conditions.
The Prescribing Question
Registered Psychologists cannot prescribe medication in Canada. Their training focuses on psychological interventions—therapy, behavioural strategies, and skill-building - rather than medical treatments.
This limitation actually strengthens treatment for many people. Research on integrated care models shows that when Registered Psychologists provide therapy while collaborating with physicians or psychiatrists for medication management, depression response rates improve from 40-45 percent with usual care to 60-70 percent with coordinated treatment.
Think of it this way: A person struggling with panic attacks sees their Registered Psychologist weekly for exposure therapy and cognitive restructuring. The psychologist coordinates with their family physician or psychiatrist who manages medication, adjusting dosages based on the psychologist's detailed observations of panic frequency and therapeutic progress between medical appointments.
This collaborative approach combines the strengths of both professions - ongoing therapeutic support from the psychologist, medical expertise from the physician or psychiatrist.
Where This Training Applies
Registered Psychologists work in diverse settings: private practices, hospitals, community mental health centres, universities, and specialty clinics. The graduate training provides flexibility to adapt evidence-based treatments across different environments and populations.
This foundational understanding of what Registered Psychologists are - and what distinguishes them from other mental health professionals - sets the stage for exploring what they actually do in practice.
Core Psychologist Duties & Responsibilities
Registered Psychologists wear multiple professional hats throughout their workweek.
The primary responsibilities include:
Assessment and evaluation: Clinical interviews, behavioural observations, and psychological testing
Diagnosis: Using DSM-5-TR criteria and clinical judgment to identify mental health conditions
Evidence-based treatment: Individual, couples, family, and group therapy
Treatment planning: Collaborative goal-setting with clients
Progress monitoring: Tracking symptom changes and treatment response
Professional consultation: Coordinating with psychiatrists, physicians, and other professionals
Supervision: Training provisional psychologists and other professionals
Research and scholarship: Contributing to the field's evidence base (varies by setting)
This list might suggest neat, sequential phases. The reality is more integrated.
How Time Actually Divides
Research tracking Registered Psychologists found that direct client care - therapy and assessment combined - accounts for 40-50% of professional time. The remainder goes to documentation, consultation, and administrative duties.
Documentation alone consumes 25-30% of work hours. Progress notes, treatment plans, and third-party billing requirements take roughly 15-20 minutes per clinical hour.
The romanticized image of psychology as primarily therapeutic conversations drastically understates the constellation of professional activities that characterize contemporary practice. Documentation, consultation, and case management represent the invisible infrastructure that supports effective treatment.
Hospital-based psychologists spend 20-25% of their time in team meetings and case consultations. Private practitioners spend considerably less - around 5% - on collaborative coordination, though they manage more business operations independently.
Assessment Never Really Stops
In my practice, assessment and treatment aren't separate phases. Even after diagnosis, I continuously assess client responses and adjust interventions based on clinical observations.
Research supports this approach: approximately 70% of therapy sessions include some form of evaluation activity, whether formal questionnaires or systematic observation of symptom patterns.
Experienced clinicians describe this as a recursive process. You're simultaneously gathering new information, testing hypotheses about what's maintaining the problem, and refining your treatment approach based on what you're learning.
This ongoing assessment allows for mid-course corrections when initial approaches aren't working - typically within 4-6 sessions rather than after months of ineffective treatment.
What Therapy With a Registered Psychologist Actually Looks Like
Most people have no idea what actually happens in therapy sessions.
The first session isn't open-ended conversation about your week. It's structured assessment with a specific purpose: gathering the information needed to help you.
The First Session: More Assessment Than Therapy
Expect 50-70% of your first appointment to focus on history and current symptoms. Your psychologist will likely use standardized questionnaires - brief measures like the PHQ-9 for depression or GAD-7 for anxiety - to establish baseline severity.
Research shows this structured approach improves treatment outcomes by 25-30% compared to unstructured intake sessions.
A typical first session includes:
Presenting concerns: What brought you to therapy right now?
Symptom details: When symptoms started, how they've changed, what makes them better or worse
Background history: Previous treatment, medical conditions, major life events
Safety assessment: Questions about suicidal thoughts or self-harm
Goal discussion: What you hope to get from therapy
You'll leave with a preliminary treatment direction, not a complete solution. That comes through collaborative planning in sessions 2-3.
Treatment Planning: Setting Specific Goals Together
Effective therapy requires concrete, measurable goals - not just "feel better." Research shows that specific goal-setting leads to 40% higher treatment completion rates.
Your psychologist might ask: "What would be different in your life if therapy worked?" The answer shapes everything that follows.
Think of someone seeking help for workplace anxiety. A vague goal like "reduce stress" becomes specific: "Give presentations without panic attacks" or "Stop avoiding my boss's emails for days."
What Ongoing Sessions Actually Involve
Sessions follow consistent structure, not aimless talking.
A standard 50-minute session typically includes:
Check-in: Brief mood assessment, symptom changes since last session (5-10 minutes)
Homework review: Discussing between-session practice (5-10 minutes)
Agenda-setting: Deciding what to focus on today (2-3 minutes)
Core work: Skills training, exposure exercises, or processing (25-30 minutes)
Summary and homework: Key takeaways and practice assignments (5-10 minutes)
Effective therapy sessions are highly structured and focused, not free-flowing conversations. Each session builds on the previous one, with clear agendas, specific skill-building activities, and between-session practice assignments that are essential to progress.
Specific Approaches in Action
Cognitive-behavioural therapy (CBT) for anxiety is interactive work, not passive listening. Your psychologist guides you through identifying anxious thoughts, examining evidence, and developing balanced perspectives. You'll practice these skills during sessions, then apply them in real situations between appointments.
EMDR for trauma involves focusing on traumatic memories while simultaneously tracking bilateral stimulation - the therapist's moving fingers, tapping, or audio tones. Most people find distress initially increases when accessing memories, then progressively decreases. Research shows average distress drops from 8-9 out of 10 to 2-3 out of 10 across a single processing session.
Exposure therapy for phobias means systematically confronting feared situations while practising anxiety management. Your heart rate and subjective anxiety typically spike 30-50% when exposure begins, then decline 40-60% by the end of each session.
In my practice, I've learned that explaining these processes upfront reduces anxiety about therapy itself. Clients often say knowing what to expect made starting treatment less intimidating.
How Progress Gets Tracked
Your psychologist monitors improvement through multiple methods:
Brief questionnaires at each session (2-3 minutes)
Tracking specific symptoms (panic frequency, sleep quality, relationship conflicts)
Your own observations about what's changing
Behavioural markers (attending avoided events, completing difficult tasks)
This systematic tracking matters. Research shows that session-by-session monitoring increases positive outcomes by 65-90% for clients who would otherwise plateau or deteriorate.
The Relationship Makes Everything Else Work
The therapeutic alliance - mutual trust, agreed-upon goals, collaborative engagement - predicts outcomes across all therapy types. Studies show it accounts for 7-10% of treatment variance, often mattering as much as specific techniques.
After years of practice, I've found the relationship is the foundation that makes skills and interventions effective. When clients feel understood and respected, they're more willing to try uncomfortable exercises and stick with treatment when progress feels slow.
This is what sets therapy apart from advice or self-help: the ongoing partnership with someone trained to notice patterns, adjust strategies, and stay steady when you're struggling.
The Specialized Function That Sets Registered Psychologists Apart
Most therapists conduct intakes. Registered Psychologists do something fundamentally different.
Psychological assessment uses standardized instruments to reveal patterns clinical interviews miss. Research shows formal testing identifies clinically significant findings overlooked in interviews in 60-80% of cases - including unrecognized cognitive issues, personality factors affecting treatment, and hidden trauma responses.
Assessment Versus Testing: Understanding the Difference
Testing means administering specific instruments. Assessment means integrating multiple data sources into a coherent clinical picture.
Think of testing as collecting puzzle pieces. Assessment is seeing how those pieces fit together - then understanding what the complete picture means for treatment.
Registered Psychologists receive extensive graduate training in administering, scoring, and interpreting psychological tests. This specialized training distinguishes them from unregulated counsellors who typically receive minimal or no formal assessment education.
When Comprehensive Assessment Happens
Comprehensive psychological assessment typically occurs in three situations:
Diagnostic clarification: When symptoms don't fit clear patterns or multiple conditions might be present
Treatment planning: To identify specific intervention targets and predict which approaches will work
Progress measurement: Establishing baseline functioning to track changes over time
A person struggling at work might assume they have depression. Testing reveals previously unidentified ADHD affecting concentration, completely changing the treatment approach.
What Different Tests Actually Measure
Cognitive tests like the WAIS (Wechsler Adult Intelligence Scale) measure reasoning, memory, processing speed, and problem-solving abilities. These identify learning differences, cognitive strengths that can support treatment, and limitations requiring accommodation.
Personality inventories like the MMPI-3 and PAI assess emotional patterns, interpersonal styles, and psychological vulnerabilities. They help distinguish between conditions that look similar - like bipolar disorder versus borderline personality disorder.
Symptom-specific measures track depression severity, anxiety levels, trauma responses, or eating disorder behaviours. These provide objective baselines and monitor change.
Neuropsychological assessment evaluates brain-behaviour relationships when cognitive problems, head injuries, or neurological conditions affect functioning.
The Multi-Session Process
Comprehensive assessment unfolds across multiple appointments. The initial clinical interview establishes rapport and identifies questions to address through testing. Testing sessions involve 2-4 hours of focused work with various instruments. The psychologist then spends several hours scoring, interpreting, and integrating results.
The feedback session often becomes the most valuable appointment. Research shows structured assessment feedback produces immediate therapeutic benefits - clients report increased self-understanding and reduced symptoms before formal therapy even begins.
In my practice, assessment feedback sessions are often transformative. Clients frequently describe them as life-changing.
Understanding why they struggle - not just that they struggle - allows people to approach treatment with clarity rather than shame.
Dr. Stephen Finn, founder of the Center for Therapeutic Assessment, explains: "What we've discovered is that psychological assessment isn't just about gathering information - it's a powerful intervention in itself. When done collaboratively, assessment creates a space where clients can see themselves more clearly and compassionately, which jumpstarts the therapeutic process."
How This Specialized Training Matters
The graduate-level training in assessment allows Registered Psychologists to work with complex presentations other providers often refer elsewhere. When someone isn't responding to standard treatment, comprehensive assessment frequently reveals why - and points toward what will actually help.
This specialized capability represents one of the clearest distinctions between Registered Psychologists and other mental health professionals.
The Educational Journey: What It Really Takes
Becoming a Registered Psychologist in Alberta requires significant educational investment - though the pathway differs from American requirements.
In Canada, Registered Psychologists can practice at the master's or doctoral level. This contrasts with many American states that require doctoral training for licensure as a psychologist.
The Foundation: Undergraduate Requirements
Most graduate programs require a bachelor's degree in psychology or a closely related field. Competitive applicants typically maintain strong GPAs and gain research or clinical experience before applying - working as research assistants, volunteering in mental health settings, or providing crisis support.
This pre-graduate experience helps applicants understand what they're committing to.
Master's vs. Doctoral Training in Canada
Two primary pathways exist to becoming a Registered Psychologist in Alberta.
| Training Level | Master's Degree | Doctoral Degree (PhD/PsyD) |
|---|---|---|
| Typical Duration | 2-3 years post-undergraduate | 4-7 years post-undergraduate |
| Supervised Hours Required | 1,600 hours (Alberta) | 1,600 hours (Alberta) |
| Research Component | Thesis typically required | Dissertation required |
| Scope of Practice | Full scope in most Canadian provinces | Full scope; may enhance certain specializations |
Both pathways lead to the same professional title and regulated status in Alberta. The College of Alberta Psychologists does not distinguish between master's and doctoral-level practitioners in terms of scope of practice.
The critical consideration is fit. Someone drawn to research and academic careers may benefit from doctoral training. Someone focused on clinical practice can often achieve their goals more efficiently through a master's program.
What Graduate Training Actually Involves
Graduate programs in clinical or counselling psychology typically require:
Core coursework: Psychopathology, assessment, therapy theories, research methods, ethics, and foundations of psychology
Practicum placements: Supervised clinical work across diverse settings
Research project: Thesis or dissertation demonstrating scholarly competence
Comprehensive exams: Testing mastery of core psychological knowledge (varies by program)
Research tracking clinical competence development finds that the transition from dependent to autonomous practice typically occurs around 400-600 hours of direct client contact.
The Financial Reality
Canadian graduate programs in psychology vary widely in funding. Some doctoral programs offer full funding with stipends, while many master's programs require students to finance their education through loans, work, or savings.
Tuition for graduate psychology programs in Canada typically ranges from $6,000-$15,000 annually for domestic students, though this varies significantly by institution and province.
Why Supervised Practice Matters
The supervised hours requirement isn't arbitrary.
I didn't feel truly prepared for complex cases until well into my supervised practice. Early on, I followed techniques rigidly and relied heavily on supervision for every decision.
The depth of training allows us to work safely with serious conditions - suicidality, trauma, psychosis - that require sophisticated clinical judgment developed only through extensive supervised experience.
"The students who thrive don't just endure the training years - they reframe challenges as skill-building opportunities, viewing difficult cases as learning experiences and research obstacles as problem-solving practice that develops the resilience sustaining entire careers." - Dr. Mitchel Prinstein, Director of Clinical Psychology, University of North Carolina
Registration: The Final Steps to Independent Practice in Alberta
Completing your graduate program is only the beginning.
Independent practice requires passing examinations, completing supervised hours, and registering with the College of Alberta Psychologists (CAP). These requirements exist to protect public safety by ensuring minimum competency standards across all Registered Psychologists.
The EPPP: Psychology's Licensing Exam
The Examination for Professional Practice in Psychology (EPPP) is used across North America, including all Canadian provinces. It now consists of two parts that assess different competency dimensions.
EPPP Part 1 tests foundational knowledge across eight content domains: biological bases of behaviour, cognitive-affective bases, social and cultural bases, growth and lifespan development, assessment and diagnosis, treatment intervention, research, and ethics. The exam contains 225 scored items administered over 4 hours and 15 minutes.
EPPP Part 2 is a skills-based examination using Clinical Simulation Exercises to evaluate applied competencies in intervention planning, cultural responsiveness, professional identification of limits, and consultation.
Approximately 70-75% of candidates pass Part 1 on their first attempt.
Alberta-Specific Requirements
Beyond the EPPP, the College of Alberta Psychologists requires:
| Requirement | Details |
|---|---|
| Supervised Practice | 1,600 hours for master's-level; requirements vary based on program type |
| Jurisprudence Module | Tests knowledge of Alberta-specific laws and CAP standards of practice |
| Continuing Competence | Ongoing requirements to maintain registration |
Always verify current requirements directly with CAP. Requirements evolve, and what applied when a colleague registered may differ from current standards.
The Provisional Psychologist Stage
During supervised practice, you hold the title of Provisional Psychologist. This allows you to practice under supervision while completing the hours required for full registration.
Most practitioners require:
Criminal record check: Including vulnerable sector screening
Professional references: From supervisors confirming competence
Documentation of training: Official transcripts and program verification
Registration fees: Annual fees to maintain CAP registration
Maintaining Your Registration
Registration isn't permanent without ongoing professional development.
CAP requires continuing competence activities to maintain active registration. This includes professional development, staying current with research and best practices, and adhering to ethical standards.
Registered Psychologists who also hold registration in other provinces need to understand differing requirements across jurisdictions.
Where Registered Psychologists Work: Career Flexibility
The profession offers remarkable career diversity.
Registered Psychologists work across settings that would seem incompatible in most careers:
Private practice: Solo or group practices providing outpatient therapy and assessment
Hospitals and health centres: Integrated care teams treating medical and mental health conditions together
Community mental health centres: Serving underserved populations with wraparound services
Universities: Counselling centres, teaching positions, and research laboratories
Schools: Educational assessments and intervention with children and adolescents
Government and correctional settings: Public health programs, forensic psychology, veterans services
Specialty settings: Rehabilitation centres, corporate consulting, Indigenous health services
Research tracking psychologists found that 40-60% change primary work settings at least once during their careers, most often moving toward greater autonomy and flexibility.
The Reality of Career Movement
Settings shape your daily work dramatically. Hospital psychologists see crisis situations and severe conditions regularly, developing rapid assessment skills and team collaboration expertise. Private practitioners build deeper long-term therapeutic relationships and develop specialized treatment approaches.
Think of someone starting in community mental health, treating diverse populations with limited resources. Five years later, they transition to private practice focusing on trauma, applying the diagnostic skills and cultural competence developed earlier while gaining scheduling autonomy and higher income.
Professional satisfaction varies significantly by setting. Research shows private practice correlates with highest satisfaction ratings, followed by university counselling centres, with community mental health and hospital settings showing somewhat lower satisfaction - though this varies considerably by individual fit and workplace culture.
Dr. Carol Goodheart, former president of the American Psychological Association, observes: "What consistently emerges is that each environment selects for and reinforces different aspects of our professional selves. Hospital psychologists become expert collaborators and rapid assessors. Private practitioners become skilled relationship builders and treatment planners. Neither is superior - they're different competency profiles shaped by setting demands."
Combining Multiple Roles
Many psychologists create portfolio careers that blend clinical work with teaching, supervision, consultation, or research. Studies show the majority of psychologists work in multiple capacities simultaneously.
These hybrid arrangements reduce burnout risk while extending career longevity. Research found that psychologists combining roles reported significantly lower burnout rates compared to those in single-track positions.
Building Specialized Expertise
The graduate training provides foundation for specialization in specific populations, treatment approaches, or conditions. You might focus on children and adolescents, older adults, trauma survivors, or couples. You could specialize in neuropsychological assessment, forensic evaluation, or consultation-liaison work in medical settings.
This specialization flexibility allows you to align your career with evolving interests rather than being locked into one path indefinitely.
I value the career flexibility tremendously. I've worked in various settings and each taught different skills and challenged me in distinct ways. Many colleagues successfully combine roles - maintaining a private practice while supervising provisional psychologists, or splitting time between hospital consultation and private assessment work.
The Reality of Clinical Work: What to Know Before You Commit
The textbooks don't prepare you for this part.
Clinical psychology involves sitting with complexity, uncertainty, and emotional weight that no amount of training fully captures. Understanding these realities helps you decide if this career fits - and prepares you for what's actually challenging about the work.
Progress Rarely Follows a Straight Line
Your client might improve steadily for months, then suddenly relapse right before a major life transition. This happens constantly.
Research on therapeutic outcomes shows that 30-40% of clients experience significant setbacks during treatment. These aren't treatment failures - they're part of how change actually works.
Think of someone recovering from depression who returns to session after three months of progress, reporting they've stopped leaving their apartment again. The therapeutic skills they learned haven't disappeared. They're navigating something underneath the depression - maybe fear of what life looks like when they're well, or grief about time lost to illness.
Your job isn't to prevent setbacks. It's to help people understand them.
The Challenges Nobody Mentions in Training
Client ambivalence presents constant complexity. People seek therapy while simultaneously resisting change because their symptoms serve purposes they don't recognize - protection from vulnerability, permission to avoid responsibilities, or familiar identity when everything else feels uncertain.
Textbook presentations almost never appear. Most people arrive with overlapping conditions - depression plus anxiety plus trauma history plus relationship problems plus chronic pain. You're constantly weighing which issue to address first, knowing that choosing wrong means losing weeks.
The emotional labour is substantial and invisible. Research tracking in-session therapist experiences found that clinicians make dozens of micro-decisions per session about emotional authenticity and self-disclosure. You're simultaneously listening, analyzing patterns, managing your own reactions, and deciding moment-by-moment what to say.
Dr. Jeffrey Kottler, Professor Emeritus of Counseling at California State University, reflects: "After five decades as a therapist, what still surprises me is how often I don't know what I'm doing. We train people as if therapy is straightforward application of techniques, but the reality involves constant uncertainty, improvisation, and tolerating the discomfort of not knowing whether you're actually helping."
Ethical Complexity You Can't Predict
Survey research with psychologists found that the vast majority encounter ethical dilemmas regularly that lack clear-cut answers. These aren't dramatic violations - they're gray areas about boundaries, confidentiality limits when safety isn't immediately threatened, or navigating cultural values that conflict with treatment approaches.
You'll face situations where helping means not intervening, where respecting autonomy requires watching someone make choices you know will cause harm, or where third-party requirements directly conflict with clinical judgment about what your client needs.
Knowing your limits becomes a daily practice. You'll regularly determine you're not the right fit for someone's needs, that a case exceeds your competence, or that you need consultation before proceeding. These aren't failures - they're sophisticated clinical judgment.
What Makes It Worth It
The rewards are profound but subtle. You witness people develop capacity they didn't know they had. You see someone who couldn't leave their house attend their child's graduation. You watch destructive relationship patterns shift after years of repetition.
These moments don't happen dramatically - they unfold gradually through dozens of sessions where nothing remarkable seems to occur, until suddenly something has fundamentally changed.
Early in my career, I felt pressure to have all the answers. I approached uncertainty as something to eliminate through better assessment or more training.
Now I understand that saying "I'm not sure, let's figure this out together" often strengthens therapy more than confident pronouncements. The most powerful work sometimes happens when I acknowledge not knowing.
This shift - from needing certainty to working skillfully with ambiguity - represents the professional growth that sustains long careers. It develops only through years of practice with hundreds of clients presenting problems no textbook fully addresses.
Essential Skills, Salary, and Career Outlook
The profession demands both technical excellence and emotional resilience.
Essential skills for success as a Registered Psychologist include:
Analytical thinking: Pattern recognition across symptoms, behaviours, and life circumstances
Interpersonal abilities: Building rapport with diverse clients and collaborating with other professionals
Emotional regulation: Managing your own reactions while holding space for others' distress
Cultural humility: Acknowledging what you don't know about clients' experiences
Observational precision: Noticing subtle changes in mood, behaviour, or thinking patterns
Research tracking clinicians found that emotional regulation and consistent self-care predict career longevity more strongly than analytical skills, with psychologists maintaining professional boundaries showing significantly lower burnout rates.
The interpersonal dimension matters more than many expect. Studies show cultural humility predicts higher client satisfaction compared to multicultural knowledge alone.
Salary Ranges: What You'll Actually Earn in Alberta
Financial realities vary dramatically by setting and experience level.
| Practice Setting | Starting Salary (CAD) | Mid-Career (5-10 years) |
|---|---|---|
| Community/Agency | $70,000-$85,000 | $85,000-$100,000 |
| Hospital/Health Authority | $80,000-$95,000 | $95,000-$115,000 |
| Private Practice | $60,000-$90,000 | $100,000-$150,000+ |
| Academic/University | $75,000-$90,000 | $90,000-$120,000 |
Private practice income varies substantially based on caseload, fee structure, and specialization. These figures represent gross income before expenses for private practitioners.
Geographic location within Canada creates income differences. Alberta typically offers higher compensation than many other provinces, though cost of living - particularly in Calgary - factors into real purchasing power.
The Financial Reality Timeline
Unlike American counterparts who often carry substantial educational debt, Canadian-trained psychologists typically graduate with more manageable debt loads due to lower tuition costs and shorter training pathways for master's-level practitioners.
Financial stability in private practice typically arrives 3-5 years after starting, as you build a referral network and establish your reputation. Agency and health authority positions offer more predictable income from the start.
Think of two new registrants: one enters a health authority position at $85,000 with predictable annual raises and benefits. Another pursues private practice, experiencing variable income for years 1-3 but eventually building a practice earning $130,000 by year five. Both paths work, but require different financial tolerance and risk appetite.
Career Outlook and Job Security
The profession shows steady demand in Alberta. Mental health awareness has increased help-seeking behaviour, while the supply of Registered Psychologists hasn't kept pace.
Licensed professionals experience strong job security. Demand exceeds supply in many areas, particularly integrated primary care, rural and remote communities, Indigenous health services, and child/adolescent specializations.
The career combines financial stability with meaningful work - and Canadian training pathways often allow practitioners to reach that stability faster than their American counterparts.
Conclusion: Is This Career Right for You?
The path to becoming a Registered Psychologist demands significant investment.
You're looking at years of graduate training, supervised practice requirements, and work that requires sitting with emotional complexity daily. Research shows that the majority of psychologists report being satisfied with their career choice - but this isn't a career for everyone, and recognizing that early saves years of investment in the wrong direction.
If You're Exploring This Career Path
Start with direct exposure before committing to graduate applications. Volunteer at crisis lines, shadow practising psychologists across different settings, or work in mental health support roles for 6-12 months. These experiences reveal whether the daily reality matches your expectations.
Think of someone who volunteers at a crisis line for three months and discovers they find the work energizing rather than draining - that's signal. Conversely, recognizing after six months that you prefer solving concrete problems over sitting with ambiguity saves you from years in misaligned training.
Research graduate programs carefully. Understand the master's versus doctoral pathways, funding structures, and specialization options. Connect with current students and recent graduates to learn what training actually involves beyond course descriptions.
If You're Seeking a Registered Psychologist
Understanding what Registered Psychologists offer helps you find the right professional for your needs.
Their specialized training in psychological assessment and evidence-based treatment makes them particularly valuable when: you need diagnostic clarification, standard therapy hasn't worked, you're dealing with complex overlapping conditions, or you want comprehensive evaluation guiding treatment.
You don't need to understand all the credentials and training differences to get help - but knowing Registered Psychologists can provide assessment and diagnosis that unregulated practitioners cannot helps you advocate for the services you need.
A Personal Reflection
This isn't an easy path. The training is demanding, the emotional labour is real, and administrative burdens can feel overwhelming.
Yet for those genuinely drawn to understanding how minds work and helping people through their most difficult moments, few careers offer comparable depth. You're present for transformations that unfold slowly, witnessing someone develop capacities they didn't believe they possessed.
Behind the credentials and specialized training, we're professionals who walk alongside people through their most challenging experiences. That represents a privilege few careers provide.
Crisis Support Resources
If you're experiencing a mental health crisis, immediate support is available:
988 Suicide Crisis Helpline: Call or text 988 (available across Canada)
Alberta Mental Health Help Line: 1-877-303-2642 (24/7)
Crisis Services Canada: 1-833-456-4566
Immediate danger: Call 911 or go to your nearest emergency room
Becoming a Registered Psychologist offers meaningful work for those willing to invest in training and emotional development. The field needs people who approach this work with realistic expectations, genuine curiosity about human behaviour, and commitment to helping others navigate psychological challenges.
Whether you're considering this career or seeking services, understanding what Registered Psychologists actually do - the specialized training, assessment capabilities, and therapeutic approaches - helps you make informed decisions about your path forward.